-
Ganesh Talkies, Kolkata
Ganesh Talkies, Kolkata
Admin
23.07.2025
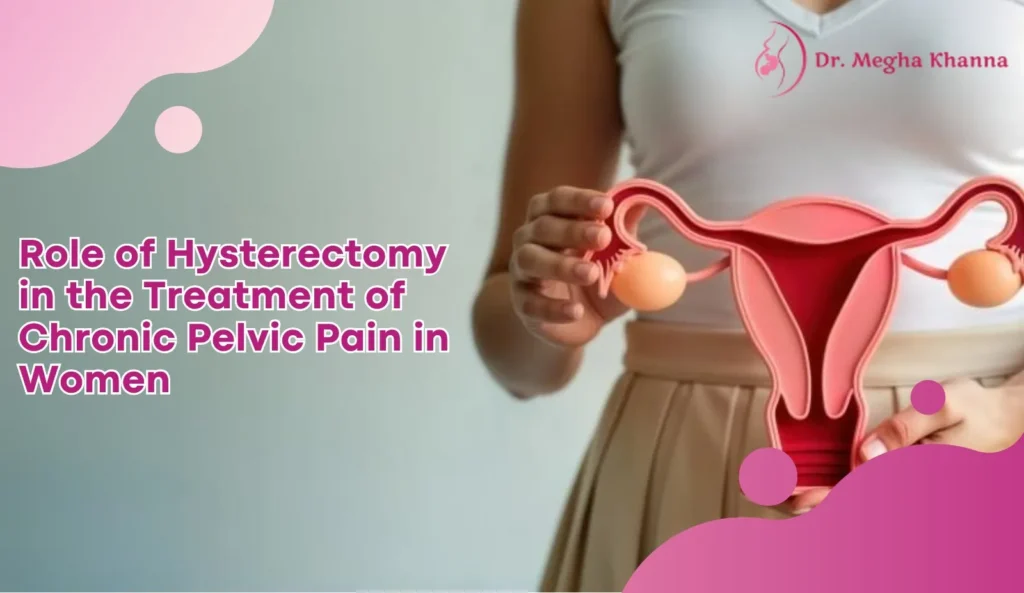
Hello Reader! Welcome to the blog page of Dr. Megha Khanna, one of the best lady gynecologist in Kolkata. Chronic pelvic pain in women is a common yet complex condition that affects millions globally. It often disrupts daily life, hampers productivity, and severely impacts emotional well-being. As one of the best gynecologists in Kolkata, I have treated countless women grappling with persistent pelvic discomfort. One of the treatment options that is often considered in severe and unresponsive cases is hysterectomy—the surgical removal of the uterus. But is hysterectomy always the answer? Let’s explore the role of hysterectomy in managing pelvic pain in women, its benefits, risks, and when it’s truly warranted. What is Chronic Pelvic Pain?Common Causes of Chronic Pelvic Pain in WomenWhen is Hysterectomy Considered?Types of HysterectomyBenefits of Hysterectomy for Chronic Pelvic PainRisks and ConsiderationsAlternatives to Hysterectomy1. What is the role of hysterectomy in treating chronic pelvic pain in women?2. Is hysterectomy always necessary for pelvic pain in women?3. Can pelvic pain persist after hysterectomy?4. What are the risks of undergoing a hysterectomy for pelvic pain?5. Who is the ideal candidate for hysterectomy to treat pelvic pain? What is Chronic Pelvic Pain? Chronic pelvic pain is defined as pain in the lower abdomen or pelvis that lasts for six months or longer. It may be: Constant or intermittent Mild to severe Related or unrelated to menstruation or intercourse This condition is not just a symptom but can be a diagnosis in itself. As the best gynecologist in Kolkata, I always emphasize a thorough evaluation before jumping to conclusions. Common Causes of Chronic Pelvic Pain in Women Understanding the root cause is essential. Some of the most common conditions causing pelvic pain in women include: Endometriosis Adenomyosis Uterine fibroids Pelvic inflammatory disease (PID) Interstitial cystitis Irritable bowel syndrome (IBS) Pelvic floor dysfunction In some cases, no identifiable cause is found, complicating the treatment strategy further. When is Hysterectomy Considered? A hysterectomy is usually not the first line of treatment. However, it is considered when: All conservative treatments (painkillers, hormonal therapy, physical therapy) have failed. The patient has a diagnosed structural cause like large fibroids or adenomyosis. The pain is significantly affecting the woman’s quality of life. The woman does not wish to have future pregnancies. Being one of the best gynecologists in Kolkata, I always ensure that my patients fully understand the nature of the surgery, its permanence, and the...

Admins
16.07.2025
Painful periods can disrupt life, but are treatable with expert care. Learn why women experience cramps and how a reputed gynecologist can help. For many women, periods are an inevitable part of life—a monthly reminder of their body’s natural cycle. But for some, menstruation comes with an added burden: painful periods that make even the simplest tasks feel overwhelming. What Are Painful Periods?Why Do Some Women Experience More Pain Than Others?Excess ProstaglandinsUnderlying Medical ConditionsAge and Hormonal FluctuationsLifestyle FactorsWhen Should You See a Gynecologist?Effective Remedies to Manage Painful PeriodsLifestyle ModificationsHome RemediesMedical TreatmentsHow to Deal With Painful Periods NaturallyAcupuncture and AcupressureDietary ChangesMind-Body TechniquesFAQs About Painful PeriodsTake Charge of Your Menstrual Health With the Right Care If you’ve ever found yourself curled up in bed with heating pads or reaching for painkillers every month, you’re not alone. It’s estimated that nearly 70% of women experience menstrual cramps at some point in their lives. But why do some women have more severe pain than others? And when should you seek help? Let’s dive into the causes, symptoms, and remedies for painful periods to help you understand your body better. What Are Painful Periods? Painful periods, also called dysmenorrhea, refer to cramping pain in the lower abdomen during menstruation. These cramps occur because of uterine muscle contractions triggered by hormone-like substances called prostaglandins. There are two main types of dysmenorrhea: Primary Dysmenorrhea: This is the most common type and is not linked to any specific health condition. It often starts in the teen years and lessens with age or after childbirth. Secondary Dysmenorrhea: This happens due to underlying medical conditions like endometriosis or fibroids and typically worsens over time. Why Do Some Women Experience More Pain Than Others? While mild cramps are normal, some women experience debilitating pain that affects work, studies, and social life. The reasons for this vary: Excess Prostaglandins High levels of prostaglandins lead to stronger uterine contractions. These contractions can compress blood vessels and reduce oxygen supply, causing pain. Underlying Medical Conditions Endometriosis: Tissue similar to the uterine lining grows outside the uterus, causing severe pain. Fibroids: Non-cancerous growths in the uterus can increase cramping and bleeding. Adenomyosis: The uterine lining grows into the muscle wall of the uterus, leading to heavy, painful periods. Pelvic Inflammatory Disease (PID): Infection in reproductive organs can cause long-lasting pelvic pain. Age and Hormonal Fluctuations Teenagers and women under 30 often have higher prostaglandin levels....

Admins
12.07.2025
The role of Vitamin D in pregnancy is vital for both mother and baby health. A reputed gynecologist can guide you in maintaining healthy levels and preventing complications for a safe journey. Vitamin D is often called the “sunshine vitamin,” but its importance goes far beyond bone health. For women during pregnancy, Vitamin D plays a crucial role in ensuring both maternal wellbeing and healthy fetal development. Why Is Vitamin D So Important During Pregnancy?Here’s why Vitamin D matters: Supports Baby’s Bone Development Strengthens Maternal Immunity Helps Prevent Pregnancy Complications Affects Long-Term Child HealthCommon Causes of Vitamin D Deficiency in Pregnant WomenThe Role of Vitamin D in Preventing Pregnancy Complications Preventing Preeclampsia Reducing Gestational Diabetes Risk Supporting Healthy Birth WeightHow to Maintain Healthy Vitamin D Levels During Pregnancy 1. Get Moderate Sunlight 2. Include Vitamin D-Rich Foods 3. Consider Supplements (if advised) 4. Monitor Levels RegularlyThe Role of Vitamin D in Boosting Maternal and Fetal HealthFAQs About Vitamin D and PregnancyBuild a Healthier Future With Optimal Vitamin D in Pregnancy In India, studies show that a significant percentage of women of reproductive age are deficient in Vitamin D. This makes understanding its impact even more essential, especially for those planning or experiencing pregnancy. This article explores the role of Vitamin D in pregnancy, its benefits, potential risks of deficiency, and practical ways to maintain optimal levels for a safe and healthy journey to motherhood. Why Is Vitamin D So Important During Pregnancy? Vitamin D functions like a hormone in the body, regulating calcium and phosphate levels critical for developing strong bones and teeth. For pregnant women, it also influences other vital systems such as immunity, mood regulation, and even glucose metabolism. Here’s why Vitamin D matters: Supports Baby’s Bone Development Ensures the fetus develops strong bones and teeth. Helps in skeletal formation during the second and third trimesters. Strengthens Maternal Immunity Reduces risk of infections that could harm both mother and baby. Helps Prevent Pregnancy Complications Low levels are linked to preeclampsia, gestational diabetes, and preterm birth. Affects Long-Term Child Health Deficiency in mothers may lead to a higher risk of asthma and allergies in children. Common Causes of Vitamin D Deficiency in Pregnant Women Even in sunny countries like India, Vitamin D deficiency is surprisingly common. Here’s why: Limited Sun Exposure: Cultural practices, indoor lifestyles, and air pollution reduce sun exposure. Dietary Gaps: Few natural food sources contain sufficient...
Admins
07.07.2025
Cervical cancer can be detected early with the right screenings. Learn how top gynecologists and healthcare experts approach early diagnosis to improve outcomes for women. Understanding Cervical Cancer: Why Early Detection MattersWhat Causes Cervical Cancer?Signs and Symptoms to Never IgnoreHow to Detect Cervical Cancer Early1. Pap Smear Test (Papanicolaou Test)2. HPV DNA Testing3. Colposcopy4. BiopsyWho Should Get Screened?How Often Should You Get Tested?What Can You Do to Reduce Risk?Role of a professional gynecologistFAQs About Cervical CancerPrioritize Prevention, Not Panic Understanding Cervical Cancer: Why Early Detection Matters Cervical cancer is one of the few types of cancer that is highly preventable and curable when detected early. Despite advancements in women’s healthcare, many women in India still miss out on timely screenings due to lack of awareness, cultural hesitation, or fear of results. But here’s the truth: Early detection doesn't just improve treatment outcomes—it can save lives. What Causes Cervical Cancer? This type of cancer develops in the cervix—the lower part of the uterus. In most cases, it's linked to persistent infection with the human papillomavirus (HPV), a common sexually transmitted infection. Not all HPV types cause cancer, but certain high-risk strains are responsible for the majority of cases. Risk factors include: Early sexual activity Multiple sexual partners Smoking Weakened immune system Long-term use of oral contraceptives Family history of cervical cancer Signs and Symptoms to Never Ignore Early stages of cervical cancer often have no noticeable symptoms. That’s why routine screening is crucial. However, as the disease progresses, symptoms may include: Unusual vaginal bleeding (between periods, after intercourse, or post-menopause) Foul-smelling or watery vaginal discharge Pelvic pain or discomfort during intercourse Lower back pain or leg swelling in advanced stages These signs should prompt immediate consultation, especially from a gynecologist with the clinical expertise and empathy needed to guide you through early detection and care. How to Detect Cervical Cancer Early Early detection largely depends on regular screening and paying close attention to your body. Here’s how you can stay ahead: 1. Pap Smear Test (Papanicolaou Test) This is the most common and effective screening tool. A small sample of cervical cells is collected and examined for abnormalities. It can detect precancerous conditions long before they turn cancerous. Recommended for women aged 21 to 65 Usually done every 3 years If combined with HPV testing, can be done every 5 years 2. HPV DNA Testing This test checks for the presence...